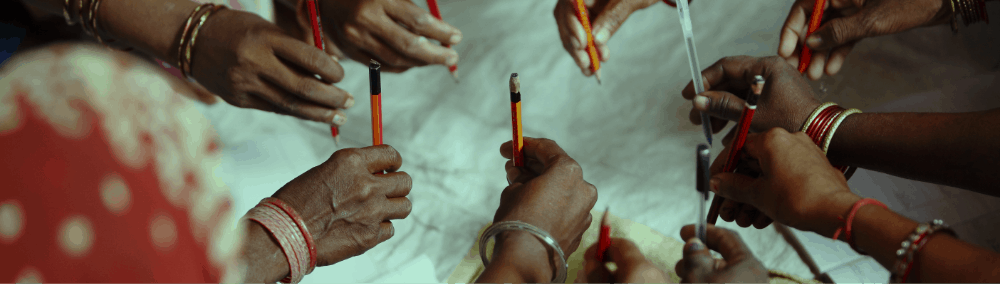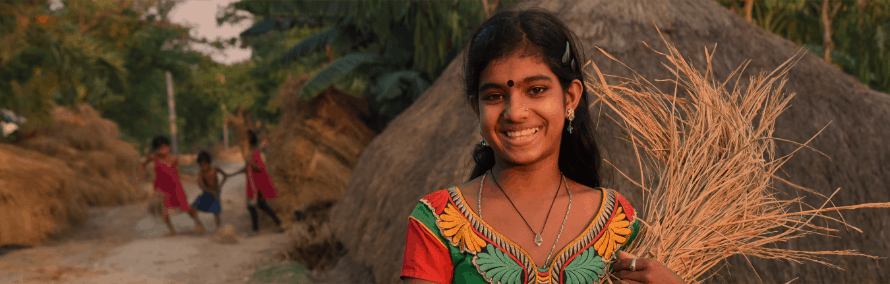The latest insight to creating impact at scale
Our Mission
We envision a more equitable future, where everyone has a chance to prosper
We envision a more equitable future,
where everyone has a chance to prosper
and we're in a hurry to get there.
0
m
Livelihoods
enabled
enabled
0
k
Micro-entrepreneurs incubated
0
k
Employees
pan-india
pan-india
0
States and 12,000+ pincodes covered
We've committed ourselves
In order to maximize our impact, build deep expertise, make results measurable, and build repeatable frameworks, we’ve kept our focus narrow. Our work focuses on improving education, ensuring health and well-being, building skills, and uplifting through employment and entrepreneurship.
We believe every success in any of these areas is a step to a more resilient future.
We believe every success in any of these areas is a step to a more resilient future.
As seen on
Previous
Next
Our partners
Previous
Next
Accolades










Empowering Women Beyond Limits
The International Women’s Day celebrated on March 8 brings together women from all walks of life to revel in a day of

March 14, 2024

Empowering Women Beyond Limits
The International Women’s Day celebrated on March 8 brings together women from all walks of life to revel in a

March 14, 2024

September 16, 2021
Bridge Over Troubled Waters
Hear from The Champion
We are very elated that through this initiative, we could support the nation’s mission to vaccinate all & protect them from COVID-19.
Tony BerlandCEO & MD, Legrand Group 
I had never dreamed I would be able to open my own garage. I have been able to earn respect as an entrepreneur, support my family, and the education of my three sisters. None of this would be possible without the support I have received.
Mohammad Kader GaziMohammad Kader Gazi 
Since the earliest days of the pandemic, Promega India has focused on keeping our employees safe and providing support to communities. We continue to explore meaningful ways to help in saving lives and are committed to support the nation in this time of crisis.
Dr. Rajnish BhartiGeneral Manager, Promega Biotech India Pvt. Ltd.